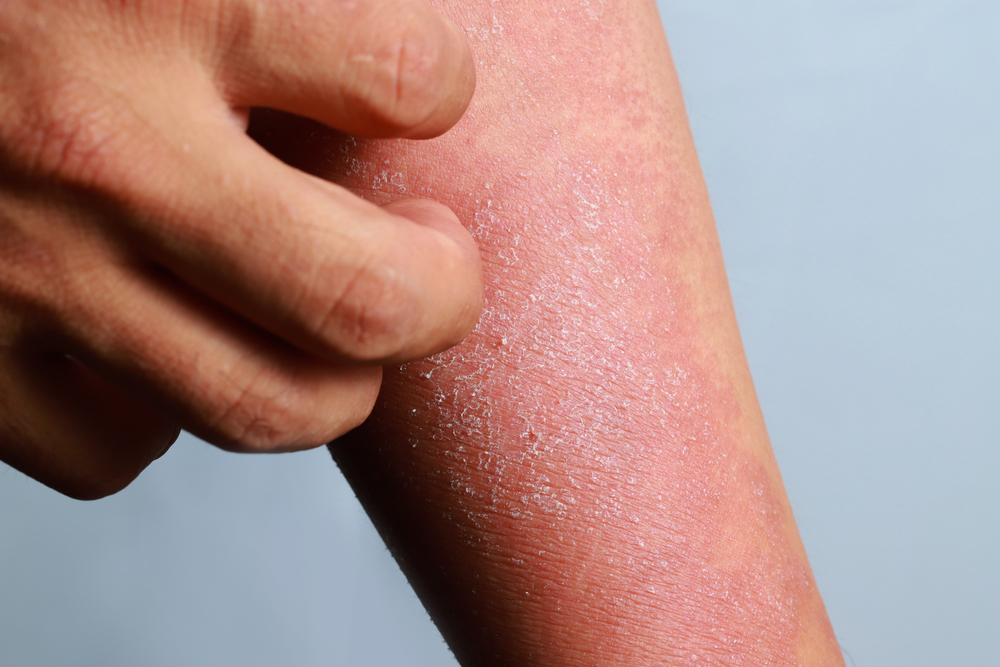
Dry, itchy, irritated skin is one of the most common but overlooked symptoms experienced by people with diabetes. For some individuals, it’s one of the earliest signs that something is wrong. For others, it shows up years after diagnosis and becomes a daily frustration.
But why does this happen? Why do diabetics have dry skin in the first place? And more importantly, what can you do about it?
To answer these questions, we need to explore how diabetes affects the body, what leads to dry or fragile skin, and how a functional medicine approach can help restore both skin health and metabolic balance.
What Is Diabetes?
Diabetes is a chronic metabolic condition that affects how the body regulates blood sugar (glucose). Glucose is one of the body’s main sources of energy, but it must be moved into cells with the help of insulin, a hormone produced by the pancreas.
Two Common Types of Diabetes
Type 1 Diabetes
- The immune system attacks insulin-producing cells in the pancreas.
- People with Type 1 need insulin to survive.
- This typically develops in childhood or adolescence but can appear later.
Type 2 Diabetes
- The body becomes resistant to insulin and struggles to use it effectively.
- Over time, insulin production may also decrease.
- It’s more common in adults but is increasingly seen in younger populations.
What Happens When Insulin Doesn’t Work Properly?
- Glucose builds up in the bloodstream instead of entering cells.
- High blood sugar leads to inflammation and damage throughout the body.
- Energy production becomes less efficient.
- Blood vessels, nerves, and hormones become stressed over time.
This multi-system impact is why diabetes affects far more than blood sugar. It influences digestion, immunity, circulation, hormones, skin health, and more.
Why Do Diabetics Have Dry Skin?
Dry skin for diabetics isn’t random; it’s a very predictable physiological response to changes caused by high blood sugar and metabolic stress.
Here are the main reasons diabetics often struggle with dry skin:
1. Poor Circulation
Chronically elevated blood sugar can damage blood vessels over time. When circulation weakens, then…
- Less oxygen and nutrients reach the skin.
- Skin repairs itself more slowly.
- The outer layers of the skin lose moisture.
This leads to the following symptoms:
- Dryness
- Flaking
- Cracks
- Slow healing
People with diabetes commonly notice dryness in the following areas:
- Legs
- Hands
- Feet
- Elbows
- Lower arms
2. Nerve Damage (Diabetic Neuropathy)
Neuropathy affects the nerves that communicate between the skin and the brain. When the nerves are weakened, then…
- Sweat glands may stop working properly.
- The body produces less natural moisture.
- Skin becomes fragile and more prone to cracking.
Dry skin caused by neuropathy in diabetics often shows up on the lower legs and feet.
3. Higher Risk of Infections
High blood sugar affects immune system function, making it harder for the body to fight off bacteria or yeast. When the skin becomes dry and cracked, then…
- Bacteria can enter more easily.
- Fungal infections (such as athlete’s foot) become more common.
- Eczema-like irritation can develop.
Infections worsen dryness, creating a cycle that many diabetics struggle to break.
4. Excessive Urination Leads to Dehydration
When blood sugar is high, the kidneys attempt to remove extra glucose through urine. This results in the following symptoms:
- Frequent urination
- Loss of fluids
- Overall dehydration
And dehydrated people have dehydrated skin.
Some diabetics drink water constantly but still feel dry—this can be a sign that blood sugar is too high for the body to stay hydrated.
5. Skin Barrier Dysfunction
Stable blood sugar is essential for a healthy skin barrier. When glucose spikes regularly, then…
- The lipid (fat) layer of the skin becomes weaker.
- Moisture escapes faster.
- Skin struggles to retain oils.
This leads to chronic dryness, especially in harsh weather or low-humidity environments such as Colorado.
6. Hormonal Imbalances
Insulin doesn’t work alone. It’s connected to other hormones such as cortisol, thyroid hormones, and sex hormones. When insulin is unstable, then…
- The endocrine system shifts out of balance.
- Oil production in the skin declines.
- Inflammation increases.
This can amplify dryness, redness, and irritation.
What Dry Skin Can Lead to in Diabetics
Dry skin may seem minor, but in diabetic patients, it can escalate into larger issues:
- Skin infections (bacterial or fungal)
- Cracks that bleed
- Ulcers, particularly on the feet
- Slow wound healing
- Itching that disturbs sleep
- Worsening neuropathy symptoms
- Increased inflammation
In severe cases, untreated skin dryness can contribute to complications that require medical intervention. This is why addressing dry skin for diabetics isn’t just a cosmetic choice. It’s a diabetes health priority.
How Functional Medicine Approaches Dry Skin in Diabetics
Functional medicine looks deeper than surface symptoms. Rather than simply treating dryness with moisturizers, it asks the following questions:
- Why is the skin dry?
- What internal dysfunction is contributing?
- What systemic imbalances need to be corrected?
Functional medicine doctors explore the root causes behind diabetes-related skin issues and build a plan that restores skin health from the inside out.
Here’s how:
1. Balancing Blood Sugar
Diabetics’ dry skin improves significantly when glucose levels stabilize. Functional medicine supports this through the following methods:
- Personalized nutrition
- Blood sugar tracking
- Lowered inflammation
- Improved insulin sensitivity
- Stress reduction
- Gut optimization
Once blood sugar becomes more stable, the skin often becomes more hydrated naturally.
2. Healing the Gut
Gut health plays a surprising role in skin hydration and inflammation. Conditions such as…
- Dysbiosis
- Leaky gut
- Food sensitivities
- Inflammatory overgrowth
…can worsen diabetic skin symptoms.
Functional medicine uses targeted strategies such as the following:
- Probiotics
- Anti-inflammatory diets
- Removal of irritants
- Digestion support
- Microbiome testing
A healthier gut often leads to healthier skin.
3. Improving Circulation
A functional medicine plan may include the following:
- Movement therapy
- Anti-inflammatory nutrients
- Cardiovascular support
- Natural herbs to support blood flow
Better circulation = healthier, more hydrated skin.
4. Restoring Hormone Balance
Since insulin resistance affects hormones, functional medicine examines the following:
- Thyroid function
- Stress hormones
- Sex hormones
- Inflammatory markers
Balancing hormones helps regulate oil production, moisture retention, and healing.
5. Supporting Hydration and Electrolytes
Sometimes diabetics drink water without absorbing it well. Functional medicine helps optimize hydration by doing the following:
- Balancing electrolytes
- Evaluating mineral deficiencies
- Reducing glucose-induced dehydration
- Assessing kidney function
This leads to better internal hydration and improved skin texture.
6. Addressing Inflammation at the Root
New research shows diabetes is heavily influenced by chronic inflammation. Inflammation also dries out the skin, disrupts repair, and weakens its barrier.
Functional medicine reduces inflammation through the following strategies:
- Dietary changes
- Identification of inflammatory triggers
- Targeted supplementation
- Stress and sleep management
- Detoxification pathways
This helps the skin rejuvenate more quickly.
Lifestyle Tips to Improve Dry Skin in Diabetes
Functional medicine emphasizes small, consistent habits that support whole-body healing:
- Drink enough water with electrolytes
- Use fragrance-free moisturizers
- Avoid hot showers
- Add omega-3 fatty acids to meals
- Skip harsh soaps
- Manage stress
- Improve sleep quality
- Keep blood sugar stable
These changes help restore moisture and support healthier skin long-term.
Functional Medicine Diabetes Care in Colorado Springs
If you’re struggling with dry skin or other symptoms related to diabetes, the team at True Life Medicine offers a thoughtful, whole-person approach to healing. Our providers uncover the root causes behind diabetes symptoms and support long-term wellness, not just symptom relief.
Learn more or schedule today at https://truelifemedicine.com/diabetes-treatment-colorado-springs.